WEEKLY BULLETIN ON OUTBREAKS
AND OTHER EMERGENCIES
Week 39: 19 - 25 September 2022
Data as reported by: 17:00; 25 September 2022
...
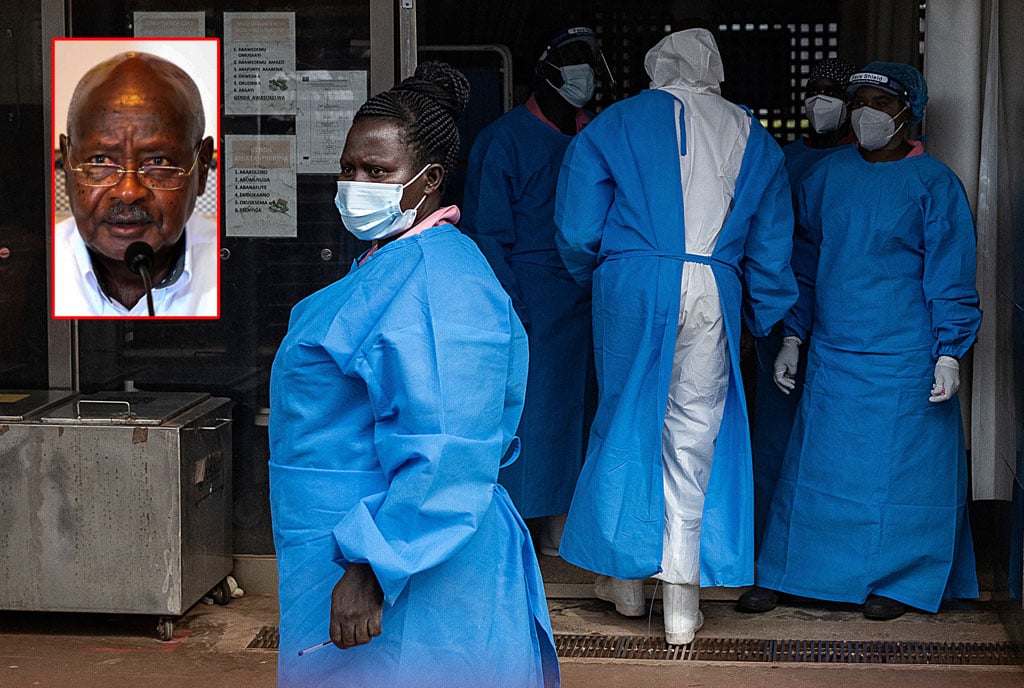
Ebola Virus Disease caused by Sudan virus in Uganda
36 cases
23 Deaths
64.0% CFR
EVENT DESCRIPTION
In line with the International Classification of Disease for
filoviruses (ICD-11) released in May 2019, outbreaks of a disease
caused by the Sudan ebolavirus are named Sudan Virus Disease
(SVD) outbreaks. This is the first outbreak of SVD since the new
classification.
On 20 September 2022, the Uganda Ministry of Health officially
declared an outbreak of SVD. The index case is a 24-year-old male
residing in Ngabano village, Madudu Sub-County in Mubende
District. His symptom onset was on 11 September, when he
developed high grade fever, tonic convulsions, blood-stained
vomit and diarrhoea, loss of appetite, pain while swallowing,
chest pain, dry cough and bleeding in the eyes.
He therefore attended two private clinics successively between
11-13 and 13-15 September without improvement. He was then
referred to the Mubende Regional Referral Hospital (RRH) on 15
September where he was immediately isolated as a suspected
case of viral haemorrhagic fever. A sample was collected on 17
September and sent to the Uganda Virus Research Institute in
Kampala where RT- PCR tests conducted were positive for SVD
on 19 September. On the same day, the patient died.
According to ongoing investigations, a series of unexplained
community deaths from an unknown illness, and sudden deaths
appearing in Madudu and Kiruma Sub-Counties of Mubende
District were reported in the first two weeks of September.
Preliminary findings revealed six other suspected deceased cases
with ages ranging from 10 days to 56 years recorded at Mubende
RRH and a few private clinics in Kiruma (five cases) and Madudu
(one case) sub-counties of Mubende district. These fatal cases
include four members of one family and one health care worker.
The deaths occurred between 1–15 September. The cases were
not isolated while in treatment and they were traditionally buried
through gathering ceremonies without specific infection control
measures.
As of 25 September 2022, a total of 36 cases have been reported
including 18 confirmed and 18 probable cases. Twenty-three
deaths have been recorded, including five confirmed, for an
overall case fatality ratio (CFR) of 64% and 28% among confirmed
cases. Women (67%) are twice more affected than men, and 37%
of cases are aged below 20 years.
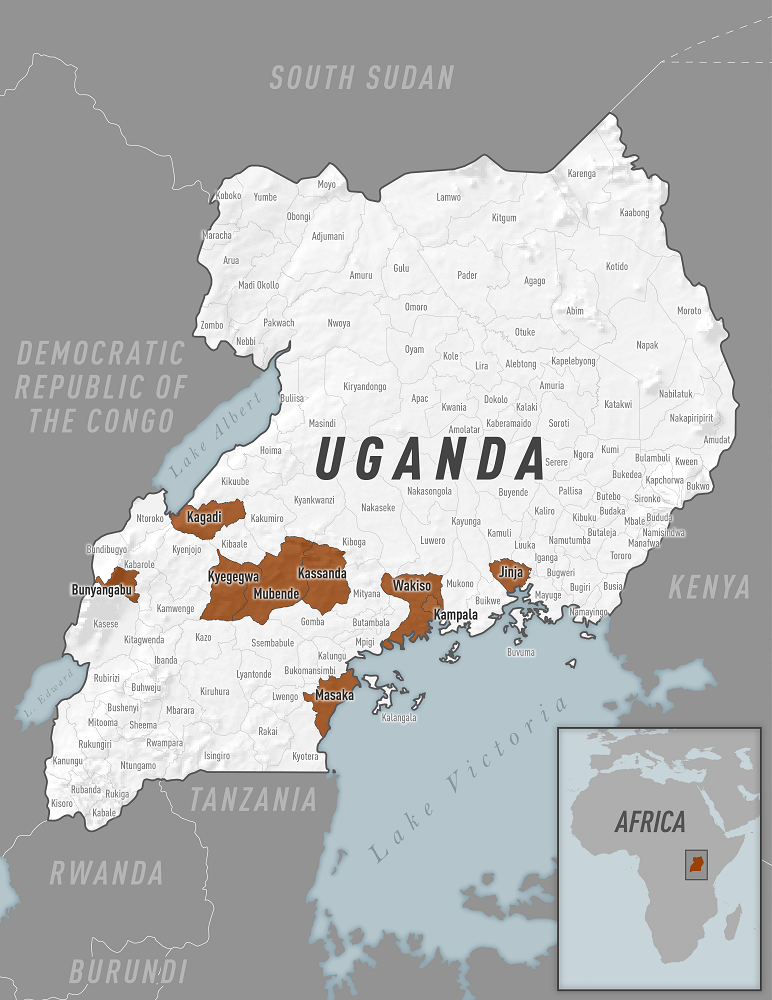
Three Districts have so far been affected: Mubende, the epicentre
with 32 cases, Kyegegwa with three confirmed casesand
Kassanda withone confirmed case. Thirty-five patients are
currently in admission including 22 suspected and 13 confirmed
cases. A total of 399 contacts have been listed with a 26% followup
rate in the past 24hrs.
PUBLIC HEALTH ACTIONS
Coordination
A National Task Force has been established by the MoH, with
WHO providing technical support, and daily meetings are
being held.
A national SVD response plan has been approved to guide
response activities.
An Incidence Management Team (IMT) has been activated
at national level and the MoH Incident Commander has been
deployed to Mubende District to support response efforts
locally. A situation room has been established at Mubende
RRH to support the coordination.
District Task Force (DTFs) meetings have been activated
in Mubende, Sembabule, Kyankwanzi, Kampala, Mityana,
Kyegegwa, Gomba, Kiboga, Kassanda, Kazo, Kakumiro and
Kibaale.
Rapid Response Teams have been deployed to the 12
districts to activate the response mechanisms, conduct risk
assessments and support development of district response
plans.
Surveillance and Laboratory
Epidemiological investigations, contact tracing, and active
case finding in the districts are ongoing. A total of 399
contacts have already been listed with 176 over the past
24hrs; 104 contacts (26%) have been followed-up. In
addition, an alert desk has been established in Mubende
District: 24 alerts have been received in the past 24hrs, 11
(46%) of which have been investigated.
The Mubende surveillance sub-committee has been activated
and briefed on its role.
Eighteen supervisors have been trained in contact tracing,
alert management, case investigation, event-based
surveillance, and data management.
Additional epidemiologists have been deployed to support
the neighbouring districts, and surveillance tools have been
printed and distributed.
Laboratory experts have been deployed from national level
and capacity building support, sample collection, packaging,
and transportation is ongoing.
Two Bio-fire mobile laboratory equipment and assorted
accessory equipment have been deployed to Mubende, with
a capacity of 20 samples to be tested per day. In an event of
increased number of samples, a higher version of Bio-fire
will be deployed.
Case management and infection, prevention and control (IPC)
Management of patients (suspected and confirmed) is
ongoing at Mubende RRH. A total of 35 patients are currently
in admission at Mubende RRH.
The case management pillar has deployed experts for IPC as
well patient care and treatment to support Mubende RRH.
Mortuary attendants have been trained in safe and dignified
burial practices.
WHO and other Partners are supporting the MoH in
establishing an Ebola Treatment Unit at Mubende RRH.
IPC teams are supporting capacity building of health workers
in IPC and the establishment of triage in all healthcare
facilities in affected districts.
Risk communication
Information, Education and Communication materials have
been reviewed and are being disseminated to affected and
high-risk districts, especially in schools, churches, and
communities at the epicentre of the outbreak. Around 1000
students and teachers of five schools have been sensitized
in Madudu sub-country.
All four radio stations in Mubende have been engaged and
initiated the airing of WHO-sponsored messages and talk
shows.
Logistics
Three Ebola disease kits and an isolation tent have been
received at the Mubende RRH to support case management,
as well as IPC items and supplies.
Fuel cards have been provided to support the mobility of
response teams on ground.
SITUATION INTERPRETATION
The source and extent of this outbreak remain to be determined.
From available information, it is possible that the event started
three weeks ago and is already generating secondary or tertiary
cases. Also, the outbreak was detected among individuals living
around an active local gold mine with a highly mobile population.
Patients presented at different facilities yielding suboptimal IPC
practices where they died and were subsequently traditionally
buried with large gathering ceremonies. In this context, the
possibility of spread to other districts and importation of cases
to neighbouring countries cannot be ruled out. Therefore, in
the absence of specific vaccines and therapeutics, the control
of this outbreak will solely rely on early detection, isolation and
management of cases, optimal IPC measures, and robust risk
communication and community engagement.
AND OTHER EMERGENCIES
Week 39: 19 - 25 September 2022
Data as reported by: 17:00; 25 September 2022
...
Ebola Virus Disease caused by Sudan virus in Uganda
36 cases
23 Deaths
64.0% CFR
EVENT DESCRIPTION
In line with the International Classification of Disease for
filoviruses (ICD-11) released in May 2019, outbreaks of a disease
caused by the Sudan ebolavirus are named Sudan Virus Disease
(SVD) outbreaks. This is the first outbreak of SVD since the new
classification.
On 20 September 2022, the Uganda Ministry of Health officially
declared an outbreak of SVD. The index case is a 24-year-old male
residing in Ngabano village, Madudu Sub-County in Mubende
District. His symptom onset was on 11 September, when he
developed high grade fever, tonic convulsions, blood-stained
vomit and diarrhoea, loss of appetite, pain while swallowing,
chest pain, dry cough and bleeding in the eyes.
He therefore attended two private clinics successively between
11-13 and 13-15 September without improvement. He was then
referred to the Mubende Regional Referral Hospital (RRH) on 15
September where he was immediately isolated as a suspected
case of viral haemorrhagic fever. A sample was collected on 17
September and sent to the Uganda Virus Research Institute in
Kampala where RT- PCR tests conducted were positive for SVD
on 19 September. On the same day, the patient died.
According to ongoing investigations, a series of unexplained
community deaths from an unknown illness, and sudden deaths
appearing in Madudu and Kiruma Sub-Counties of Mubende
District were reported in the first two weeks of September.
Preliminary findings revealed six other suspected deceased cases
with ages ranging from 10 days to 56 years recorded at Mubende
RRH and a few private clinics in Kiruma (five cases) and Madudu
(one case) sub-counties of Mubende district. These fatal cases
include four members of one family and one health care worker.
The deaths occurred between 1–15 September. The cases were
not isolated while in treatment and they were traditionally buried
through gathering ceremonies without specific infection control
measures.
As of 25 September 2022, a total of 36 cases have been reported
including 18 confirmed and 18 probable cases. Twenty-three
deaths have been recorded, including five confirmed, for an
overall case fatality ratio (CFR) of 64% and 28% among confirmed
cases. Women (67%) are twice more affected than men, and 37%
of cases are aged below 20 years.
Three Districts have so far been affected: Mubende, the epicentre
with 32 cases, Kyegegwa with three confirmed casesand
Kassanda withone confirmed case. Thirty-five patients are
currently in admission including 22 suspected and 13 confirmed
cases. A total of 399 contacts have been listed with a 26% followup
rate in the past 24hrs.
PUBLIC HEALTH ACTIONS
Coordination
A National Task Force has been established by the MoH, with
WHO providing technical support, and daily meetings are
being held.
A national SVD response plan has been approved to guide
response activities.
An Incidence Management Team (IMT) has been activated
at national level and the MoH Incident Commander has been
deployed to Mubende District to support response efforts
locally. A situation room has been established at Mubende
RRH to support the coordination.
District Task Force (DTFs) meetings have been activated
in Mubende, Sembabule, Kyankwanzi, Kampala, Mityana,
Kyegegwa, Gomba, Kiboga, Kassanda, Kazo, Kakumiro and
Kibaale.
Rapid Response Teams have been deployed to the 12
districts to activate the response mechanisms, conduct risk
assessments and support development of district response
plans.
Surveillance and Laboratory
Epidemiological investigations, contact tracing, and active
case finding in the districts are ongoing. A total of 399
contacts have already been listed with 176 over the past
24hrs; 104 contacts (26%) have been followed-up. In
addition, an alert desk has been established in Mubende
District: 24 alerts have been received in the past 24hrs, 11
(46%) of which have been investigated.
The Mubende surveillance sub-committee has been activated
and briefed on its role.
Eighteen supervisors have been trained in contact tracing,
alert management, case investigation, event-based
surveillance, and data management.
Additional epidemiologists have been deployed to support
the neighbouring districts, and surveillance tools have been
printed and distributed.
Laboratory experts have been deployed from national level
and capacity building support, sample collection, packaging,
and transportation is ongoing.
Two Bio-fire mobile laboratory equipment and assorted
accessory equipment have been deployed to Mubende, with
a capacity of 20 samples to be tested per day. In an event of
increased number of samples, a higher version of Bio-fire
will be deployed.
Case management and infection, prevention and control (IPC)
Management of patients (suspected and confirmed) is
ongoing at Mubende RRH. A total of 35 patients are currently
in admission at Mubende RRH.
The case management pillar has deployed experts for IPC as
well patient care and treatment to support Mubende RRH.
Mortuary attendants have been trained in safe and dignified
burial practices.
WHO and other Partners are supporting the MoH in
establishing an Ebola Treatment Unit at Mubende RRH.
IPC teams are supporting capacity building of health workers
in IPC and the establishment of triage in all healthcare
facilities in affected districts.
Risk communication
Information, Education and Communication materials have
been reviewed and are being disseminated to affected and
high-risk districts, especially in schools, churches, and
communities at the epicentre of the outbreak. Around 1000
students and teachers of five schools have been sensitized
in Madudu sub-country.
All four radio stations in Mubende have been engaged and
initiated the airing of WHO-sponsored messages and talk
shows.
Logistics
Three Ebola disease kits and an isolation tent have been
received at the Mubende RRH to support case management,
as well as IPC items and supplies.
Fuel cards have been provided to support the mobility of
response teams on ground.
SITUATION INTERPRETATION
The source and extent of this outbreak remain to be determined.
From available information, it is possible that the event started
three weeks ago and is already generating secondary or tertiary
cases. Also, the outbreak was detected among individuals living
around an active local gold mine with a highly mobile population.
Patients presented at different facilities yielding suboptimal IPC
practices where they died and were subsequently traditionally
buried with large gathering ceremonies. In this context, the
possibility of spread to other districts and importation of cases
to neighbouring countries cannot be ruled out. Therefore, in
the absence of specific vaccines and therapeutics, the control
of this outbreak will solely rely on early detection, isolation and
management of cases, optimal IPC measures, and robust risk
communication and community engagement.










Comment